By DAVID J. HILL
In the summer of 2006, John Syty and his Clarence High School teammates geared up for the high school football season at a seven-on-seven passing camp in Rochester, N.Y. Syty and a teammate were running full speed in the same direction trying to intercept a pass when they collided, smacking heads. The impact knocked Syty out.
“That was by far the worst concussion I’ve had. It took about three or four hours afterward for it to click and me to start realizing what had happened,” Syty recalls. “I had no idea where we were, I had no idea what the field looked like, nothing—it was freakish. It was weird.”
It was the first of seven concussions Syty would experience as a high school and collegiate athlete.
A talented defensive player, Syty enrolled at the University at Buffalo in fall 2007 and earned a spot as a walk-on with the UB Bulls football team. Syty—the name is pronounced like “city”—made two interceptions in his first collegiate game, on Aug. 30, 2007, when the Bulls pummeled the University of Texas-El Paso 42-17 before a crowd of more than 16,000 fans in UB Stadium.
Syty continued to play well over the next few seasons, helping the Bulls win the Mid-American Conference Championship in 2008 and earning a bid to a bowl game that season. Moreover, he was the first recipient of the 1958 Lambert Cup Team Football Scholarship. The scholarship is awarded in honor of the historic Bulls team that stood up to racism when it rejected a bowl game invitation to play Florida State in Orlando, Fla., upon learning that two of UB's black players would not be permitted to play.
After a solid showing in spring camp, Syty, as a senior, was projected to start the 2011 season at middle linebacker.
“There’s no such thing as a minor concussion, and the problem is that once you have one or two, you’re more likely to have a third, fourth or a fifth, and then you are at risk for sustaining cumulative and permanent damage over time.”
—Dr. John Leddy, associate professor of clinical orthopedics and director, UB Orthopaedics and Sports Medicine Concussion Clinic
But during summer workouts, post-concussion symptoms surfaced. He experienced spells of dizziness and blurred vision. He later would learn that he also had a herniated disc in his neck. Team doctors evaluated Syty carefully after each head injury to ensure his safety; each time, Syty passed. When the symptoms crept up before his senior season, however, team physicians advised Syty that it may no longer be safe for him to play.
Post-concussion symptoms have sidelined athletes for decades, but only recently has the issue captivated the public’s attention, partially because of more advanced medical research. Largely, though, it’s because several high-profile athletes have suffered concussions, including, most recently, Buffalo Sabres goaltender Ryan Miller, one of the top netminders in the National Hockey League.
“It’s really gotten press in the last two or three years at the NFL level and NHL level. And then when you have very prominent athletes like Sidney Crosby and Eric Lindros—they get a lot of publicity and it starts to get media attention,” says John Leddy, associate professor of clinical orthopedics and director of the UB Orthopaedics and Sports Medicine Concussion Clinic, which is housed in Farber Hall on UB's South Campus, with a satellite office in Niagara Falls.
Leddy ran Syty through a battery of tests, including one in particular—an exercise-based assessment procedure in which the athlete works out on the treadmill—he developed with his colleague, Barry Willer, the clinic’s research director and a professor in the School of Medicine and Biomedical Sciences Department of Psychiatry.
The UB researchers’ graded exercise test has gained national attention, with major media outlets such as The New York Times, Boston Globe and NPR reporting on it. Willer also has been quoted in pieces by both the Times and NPR on body checking in youth hockey.
Leddy’s and Willer’s treadmill-based test has helped athletes and team doctors around the country better understand concussions and, more importantly, when it is safe for an athlete to return to play. Prior to this breakthrough, there hadn’t been a standardized test to measure when it’s safe for an athlete to return. Instead, the decision was often a judgment call by a team physician.
In Syty’s case, he had to accept a difficult certainty: it was time to hang up his helmet and leave the game of football before sustaining more severe, potentially life-altering, damage to his brain and his body. As often is the case in a patient with multiple concussions, Syty also had a neck injury.
“John had multiple concussions and neck injuries that left him vulnerable to even the slightest trauma,” explains Leddy.
Leddy and Willer have focused their research on the more severe concussion cases, individuals like Syty who fall into the approximately 10 percent of patients whose symptoms linger for more than three to six weeks. Oddly, Syty’s symptoms subsided shortly after the injury, until the seventh one.
Calling an Audible
John Syty ’11 (BS, business administration) joined the UB football team in 2007 as a walk-on. Improving after each of his first three seasons, the Clarence, N.Y., native was projected to start at middle linebacker for the Bulls for the 2011 season, his last. But the lingering effects of at least seven known concussions forced Syty to hang up his helmet or risk further, more severe, damage.
“The unique thing is, whenever I had a concussion, no matter how bad it was—headaches, throwing up, whatever—the next day I’d wake up and I’d feel perfectly fine,” Syty says. “The only thing I maybe would have is a little sensitivity to light. Other than that I felt good.”
But as summer 2011 practices ramped up, Syty’s symptoms returned, taking him by surprise. “Everything was fine. I had a really good summer, started off camp real well. For the first week, two weeks, everything was good and I was going to start at middle linebacker,” he says. “And then it just started going downhill. I just started feeling awful, to say the least.”
Syty was determined to fight through the symptoms, hoping for the best. “I tried dealing with it for a week or so, hoping it was going to go away but it wasn’t, it was getting worse so it was kind of a decision I made on my own,” he recalls. “I talked to my dad about it. I walked into coach [Jeff] Quinn’s office before practice one day and just told him what was going on and how I was feeling.”
And with that, Syty’s career as a football player came to an end, just weeks before the start of his senior year of eligibility. Coach Quinn supported Syty’s decision. Syty, who received his bachelor’s degree in business administration last spring, has stayed on with the Bulls as a volunteer coach, working with the UB linebackers and assisting with other on-field duties on game days. In addition, he is participating in an internship with the Division of Athletics.
While it’s difficult to watch from the sidelines, he knows he made the right decision. “I want to be able to have a family and have a job and hopefully be all right down the road,” he says.
“My last practice, I made a tackle and I just kind of blacked out on the tackle,” Syty recalls. “That was the day that I really just said, ‘Man, if I can’t make a tackle without even hitting my head and it’s still going to happen…’”
He pauses, then adds, “I had a good run. That’s the other thing I looked at. I accomplished everything I wanted to accomplish. I earned a scholarship, played three good seasons, won a MAC championship, went to a bowl game. I really didn’t have anything to gain. It was more just to lose.”

John Syty '11 played three years for the UB Bulls football team before deciding to end his career due to post-concussion symptoms. He currently serves as a volunteer coach.

Pro athletes bring concussions to the forefront
The professional hockey season began in October, minus one of the game’s brightest stars—Pittsburgh Penguins forward Sidney Crosby, who suffered a concussion last January that forced him to miss 10 months of action. Crosby announced in September that he wasn't going to return until fully healthy. He returned to the lineup on Nov. 21, after missing more than 60 games.

Researchers in the UB Orthopaedics and Sports Medicine Concussion Clinic developed a treadmill-based test that helps team physicians reliably determine when it is safe for an athlete to return to play after suffering a concussion.
His cautious approach is not uncommon these days. As researchers like experts at the UB Concussion Clinic learn more about how concussions impact an athlete’s performance on and off the field, team doctors are acknowledging the severity of brain injuries.
One stunning development came in October 2011, when news outlets reported that former Buffalo Sabres great Rick Martin, who died of a heart attack in March at age 59, had the same degree of trauma in his brain as other former NHL players who died fairly young.
The shocking difference was that Martin, a member of the famed French Connection line, was the first non-fighting hockey player whose postmortem identified neurodegenerative brain damage called chronic traumatic encephalopathy (CTE). A finesse player who didn’t have a reputation as a fighter, he was known to have sustained only one concussion during his 13-year NHL career.
Weeks after this development came a report that Cookie Gilchrist, the legendary Buffalo Bills running back from 1962 to 1964 who was known for his hard-nosed style of play, also had severe damage to his brain. He died last January at age 75.
Serious head injuries aren’t limited to pro athletes. As reported in September by the Canadian news service QMI Agency, Drew Wood, of Ontario, was forced to quit hockey after suffering six hockey-related concussions. He was just 16. In November, UB Neurosurgery announced a partnership with Dent Neurological Institute and the Buffalo Sabres Alumni to create a program, called PUCCS, that raises awareness of concussions in young athletes.
‘No such thing as a minor concussion,’ UB researcher says
For decades, athletes would return to action after suffering a concussion, oftentimes only moments after sustaining the injury, under the long held belief that it wasn’t a serious injury requiring a certain degree of caution. Pro Football Hall of Fame quarterbacks Jim Kelly and Troy Aikman both suffered multiple concussions throughout their careers, with Aikman experiencing 10.
“When I was playing high school sports, people went into play after concussions,” says John Leddy, associate professor of clinical orthopedics and director of the UB Orthopaedics and Sports Medicine Concussion Clinic. “Nobody realized that they were dangerous. They thought you got your ‘bell rung,’ and then you got over it and that was it.”
It’s a dangerous mindset to have, researchers say.
“There’s no such thing as a minor concussion, and the problem is that once you have one or two, you’re more likely to have a third, fourth or a fifth, and then you are at risk for sustaining cumulative and permanent damage over time,” Leddy adds. “The brain is a unique organ. You only have one, and you need it for almost everything else. Clearly, the animal and human research shows that if somebody goes back before they’re fully recovered, they’re going to fare much worse and often will have a second, more significant, injury.”
Among the professional athletes UB’s Concussion Clinic has helped is former Buffalo Sabres center Tim Connolly, now with the Toronto Maple Leafs. Leddy and colleague Barry Willer, professor of psychiatry and research director of the UB Concussion Clinic, helped Connolly return to the lineup in time for the start of the 2007 NHL playoffs, after Connolly missed the previous 11 months with post-concussion syndrome.

Treating concussion as a physiologic, rather than cognitive, issue
Notion-shattering research of the kind Leddy and Willer are doing has made a huge difference in the way team physicians and athletes look at concussions, and in addressing the challenging question of when an athlete who has sustained a concussion can return to play.
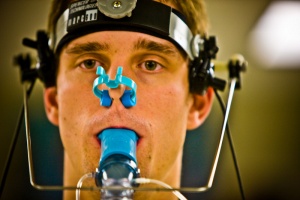
Patients at UB's Concussion Clinic are run through a battery of tests that aid in the evaluation process.
“Although there are a number of components to their decision, the most significant one is, the player is capable of returning to play when they can exercise to the level of their sport without exacerbation of symptoms,” Willer says.
“All we’re doing is assessing that systematically. So rather than take Sidney Crosby and ask him to go skate around the ice for a little while and see whether he feels OK, you put him on a treadmill and you can see exactly where he has symptom exacerbation.”
Leddy and Willer have employed the Balke treadmill protocol, a simple test during which the athlete increases the treadmill incline by a specific rate every minute and exercises until the point at which his or her concussion symptoms (headache, for example) become more severe.
Using the treadmill test team physicians can determine whether an athlete is ready to return to play. Here’s an example of how it works:
Let’s say an athlete’s maximum heart rate during physical activity is supposed to be around 200 and the athlete reaches a heart rate on the treadmill of 180 before having to stop due to worsening symptoms. At that point, doctors can determine that the athlete is close to being able to return, but he or she still should not do so. If, however, the athlete stops at a heart rate of 150, doctors know the athlete needs additional recovery time.
Research shows that within the first three weeks after a concussion, the best prescription is to rest and limit mental and physical stimuli. Until recently, team physicians largely believed that for athletes with prolonged recovery following a concussion, the best recourse was still no exercise at all for an extended period of time. But Leddy’s and Willer’s research shows that a controlled exercise program, based upon the results of the treadmill test, is actually beneficial for those whose symptoms persist beyond three weeks.
Positive results on the treadmill test can also provide a much-needed boost for the recovering athlete. “They’re enthused, and they want to get better,” says Willer.
Based on the UB research, team physicians from around the country are beginning to change the way they manage athletes who have suffered a concussion.
“It’s slowly getting there,” Willer says. “It’s a mind shift change that we’re asking for. It’s more than just convincing people that our procedure works. It really requires them to change their mindset.”
That’s because most concussion treatment programs are driven solely by neuropsychological test data. Says Willer, “That’s the issue—that it’s an issue of cognition. But the basic problem is of a physiologic nature and therefore the treatment tends to make more sense to be more physiologic.”
Leddy adds, “We feel that the best method of determining when athletes are really ready to go back and play sports to maximum intensity is the treadmill test, because the exercise test replicates the physiology of what athletes have to do during sport.”
Willer and Leddy recently gave presentations on their controlled exercise regimen at the North American Brain Injury Society conference in New Orleans, and at the American Congress of Rehabilitation Medicine conference in Atlanta. Leddy also has been contacted by a group of small Division III colleges in the New England area looking to send some of their staff to Buffalo to see how the procedure works.
A key staff member of UB’s Concussion Clinic will be training staff at Yale. “We know there are other sports medicine programs using our approach and if we learn of them we offer free training thanks to a grant from the Robert Rich Family Foundation,” Willer says.
A NOVEL APPROACH
WAYS TO GIVE
Concussion Q&A
What exactly is a concussion, and what happens to a person’s body and brain during a concussion? Barry S. Willer, professor of psychiatry and research director of the UB Orthopaedics and Sports Medicine Concussion Clinic, explains in this quick Q&A.
What is a concussion?
A concussion is defined as an altered state of consciousness resulting from an external trauma. This definition is under review because of the more recent evidence that blows to the head that appear to cause little if any alteration of consciousness, called sub-concussive blows, may cause long term damage if they occur in sufficient frequency and over a short period of time. The evidence for this is the recent reports on brain damage called CTE, chronic traumatic encephalopathy.
What happens to the brain/body during a concussion?
When someone experiences a concussion, there is an immediate set of metabolic changes referred to as a cascade. The metabolic cascade leads to some of the immediate symptoms, such as the inability to store memories, called amnesia. The cascade also causes the blood vessels of the brain to contract thus reducing the flow of blood to the brain. Over the next few hours the cascade also produces symptoms like confusion, dizziness, headache and sensitivity to light.
What’s important to know about concussions?
No two concussions are exactly the same, but most physicians and team trainers can pretty well recognize a concussion when it happens. The athlete can also recognize when a concussion happens and those of us in the field of concussion are encouraging athletes to stop hiding their symptoms and enlisting teammates to point out any unusual behavior with someone who may have received a blow to the head. It is the second blow to the head before the first concussion has healed that appears to cause the most damage. Most concussions take seven days to heal completely, although sub-concussive blows take less time.
UB FACULTY EXPERTS

John J. Leddy
Associate Professor of Clinical Orthopedics; Associate Director of University Sports Medicine

Barry S. Willer
Professor, Department of Psychiatry; Research Director, UB Orthopaedics and Sports Medicine Concussion Clinic


