
Doctoral student Tyler Rolland took the People’s Choice Award for his entry in the 2023 Art of Research competition. The blue, green and red are fluorescent color probes to visualize proteins within tissue sections on a microscope. Blue = nucleus; green = alpha-smooth muscle actin; red = fibronectin; white * = healthy/quiescent fibroblast; white # = activated/diseased fibroblast.
Jacobs School Scientists Excel in Art of Research Event
Published June 30, 2023
Researchers in the Jacobs School of Medicine and Biomedical Sciences figured prominently in the 2023 Art of Research competition carried out by The Graduate School at the University at Buffalo.
Doctoral Student Wins People’s Choice Award
Tyler Rolland, a trainee in the doctoral program in physiology and biophysics, won the People’s Choice Award for his entry titled “Duality of Cardiac Fibroblasts in Heart Health and Disease: Beneficial or Detrimental?”
Cardiac fibroblasts are cells within the heart that play a crucial role in maintaining structural integrity and proper organ function.
In a healthy heart, small spindle-shaped cardiac fibroblasts persist in a quiescent state, waiting for cues to become activated. This activation can occur rapidly following an injury to the heart, such as a myocardial infarction (heart attack), upon which cardiac fibroblasts proliferate and produce extracellular matrix proteins.
“The deposited matrix proteins provide structural support and help stabilize the damaged area, thereby maintaining the heart’s structural integrity and preventing deterioration of cardiac function,” Rolland says. “While this pattern of cardiac fibroblast activation is beneficial after injury, certain adverse stimuli can elicit inappropriate activation of fibroblasts, leading to excessive secretion of extracellular matrix proteins, formation of scar tissue, and an increase in the mass of the heart.”
The development of scar tissue leads to stiffening of the heart chambers, which interferes with normal cardiac function by compromising the heart’s ability to efficiently fill with blood between beats.
These structural changes may also compromise the reparative response to subsequent cardiac stressors, potentially leading to an increased risk of heart failure. Thus, depending on the situation, activation of cardiac fibroblasts can be either beneficial or detrimental to the heart.
“In the short term, their activation is essential in the repair process following a heart attack, but in the long term, it can contribute to the development of heart failure,” Rolland says. “Consequently, research designed to improve our understanding of factors that regulate cardiac fibroblast behavior is essential to understand the natural reparative capabilities of the heart, as well as identifying potential therapeutic targets to optimize cardiac health across the lifespan.”
Trio of Researchers Capture 3D Award
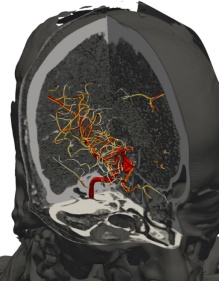
Three persons contributed to the Best 3D Rendering Award with their effort “Colors for Doctors: AI Tools for Rapid and Informative Brain Vessel Assessment.”
Tatsat Rajendra Patel, PhD, and Sricharan Veeturi, PhD, both postdoctoral associates in neurosurgery, were involved in the research with Munjal Purnkant Shah, PhD, a research assistant at the Canon Stroke and Vascular Research Center.
Stroke is a phenomenon wherein the blood pumped by the heart fails to reach certain parts of the brain. This is a deadly condition that claims more than 6.5 million lives every year. Of the individuals who survive, the vast majority are faced with lifelong disability or paralysis. Thus, timely treatment is paramount to prevent death and improve quality of life. As soon as a patient experiencing stroke symptoms is admitted to the hospital, they undergo a brain scan, such as a computered tomography (CT) or medical resonance (MR) imaging so doctors can observe the severity and location in the brain where the stroke is occurring. However, currently available techniques are non-intuitive and give limited answers.
“Our research leverages the power of artificial intelligence (AI) and image processing to give doctors a better visualization of the brain vessels and the blood flowing through them,” the researchers say. “Generally, medical images like CT or MRI are stacks of 2D pictures, which gives the doctors limited understanding of the 3D vessels in the brain. We use AI to transform these 2D pictures into a 3D model of the brain vessels which can help the doctors in better visualization.”
“In addition to this 3D rendering, we also use image analysis and blood flow simulations to estimate the blood flowing through the vessels and pinpoint potential stroke locations which can help the doctors make faster and accurate decisions, thus helping to save patient lives,” they add.

