Research Areas
Stem cells are a key component of regenerative medicine, as they open the door to new clinical applications. Our regenerative medicine faculty are studying a variety of stem cells. Contributions include engineered tools for systems biology analysis of stem cells, biological discovery, drug delivery and biomaterials, and bioengineered products for translational medicine.
Applications of Stem Cells in Regenerative Medicine
The biotechnological applications of pluripotent stem cells(PSC) include gene and cell therapy, tissue engineering, human-on-chip applications, human product production, cloning, stem cell reprogramming, personalized medicine, gene editing, assisted reproduction, understanding congenital disease, human genetic and epigenetic studies, disease modeling, chimera organism formation, drug development, and food production. One of the goals of stem cell engineering is to generate pure, homogenous, and abundant amounts of critical lineages, like cardiomyocytes, neurons, or hepatocytes. In molecular imaging, molecular biological processes, such as gene expression, receptor upregulation, and metabolism, are assessed noninvasively and quantitatively in the intact living subject. Thus, merging molecular imaging and stem cell-based disease modeling could lead to the discovery of new disease mechanisms, and new classes of molecular imaging agents that can be clinically translated as real molecular diagnostics for use in patients with diseases.
Investigators
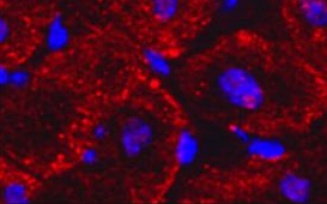
Cardiovascular Stem Cells
Scientists in the Division of Cardiovascular Medicine are evaluating the role of stem cells in preventing cardiac fibrosis and stimulating cardiomyocyte regeneration. Ongoing investigations focus on the beneficial effects of cardiosphere-derived cells (CDCs) and mesenchymal stem cells (MSCs). Both platforms stimulate endogenous myocyte proliferation while preventing myocyte cell death. We are optimizing cell delivery using widespread intracoronary administration to the entire heart as well as employing epicardial stem cell sheets to effect cardiac repair. Additional research evaluates the role of cardiosphere-derived exosomes as a cell-free paracrine mediator of cardiac repair. Our work uses translational preclinical models of viable dysfunctional myocardium and postinfarction left ventricular remodeling that can provide the pivotal research needed to move basic stem cell research into early phase clinical trials.
Investigators
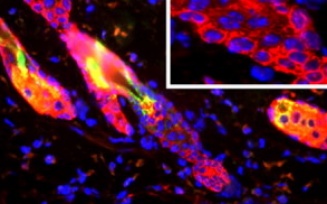
Epidermal Stem Cells
Stem cell research for Epithelial cells spans multiple organs and tissues with focus on the epidermal cells of the skin and other stratified tissues. This includes fundamental studies of mechanisms of various facets of stem cell biology including cell fate, lineage choices and differentiation using cell and organ culture as well as genetically engineered mouse (GEM) models. The research utilizes sophisticated state of art genomic, epigenomic and molecular techniques to define and identify markers for stem and progenitor sub-populations and to determine the locations and functional contributions of the different stem cell niches. The broader goals of the collaborative efforts are to map the regulatory pathways of epidermal stem cell proliferation and differentiation during development and disease such as inflammation and cancer and to utilize such knowledge for stem cell based therapies.
Investigators
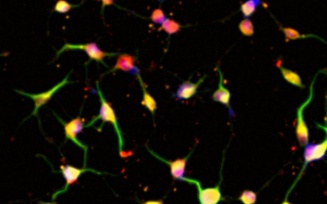
Induced Pluripotent Stem Cells & Reprogramming (iPSC and hESC)
In 2006, scientists found an alternative strategy to generate pluripotent stem cells, which they termed induced pluripotent stem cells (iPSC). They found that any somatic cell can be fully reprogrammed by introducing four pluripotency-associated transcription factors (TF): Oct3/4, Sox2, Klf4 and c-Myc. Generating iPSC does not require human egg destruction, and could be personalized for an individual so that no immune barrier exists. iPSC can also be used to study personalized disease models, such as genetic diseases, and for in vitro drug development. In a landmark study in 2014, the first patient received their own, personalized iPSC-derived cells in surgical procedure for macular degeneration. For these reasons, iPSC are a powerful tool in stem cell engineering.
Investigators
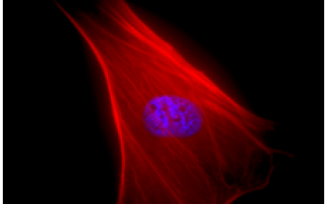
Mesenchymal Stem Cells
Mesenchymal Stem Cells (MSC) are cells of mesodermal origin that were originally isolated from bone marrow and were thought to support and maintain the hematopoietic stem cell niche (bone marrow stroma cells). Subsequently, MSCs have been isolated from different tissues, including bone marrow, adipose tissue, hair follicles, muscle, lung, spleen, and liver. These adult stem cells are multipotent as they can be coaxed to differentiate into fat, bone, cartilage and muscle; they also exhibit anti-inflammatory and are known to secrete trophic factors that promote angiogenesis and tissue regeneration in vivo. For these reasons, MSC have been widely investigated for clinical use in over 200 clinical trials to treat various conditions including cardiac diseases, neurological disorders, inflammation, brain and spinal cord injury, kidney, skin. At UB, several SCiRM investigators are studying various aspects of MSC biology as well as developing novel strategies for using MSC in regenerative medicine.
Investigators
Neural Stem Cells
Neural stem cell research focuses on understanding of the cellular and molecular events that regulate the development of the human brain. The brain is the most complex organ in the human body and is comprised of a diverse population of highly specialized neurons and glial cells. When these cells are lost or their function becomes impaired, deficits in cognitive, behavioral, sensory and motor symptoms result. Both primary neural stem cells and induced pluripotent stem cell-derived cells can be utilized to model these disease processes in the dish. Furthermore, neural stem cells and more restricted progenitor populations such as oligodendrocyte progenitor cells are promising cell therapeutic agents which can restore lost function when transplanted into animal models of disease. Research in this area involves various techniques and disciplines that encompass genomic, epigenomic, molecular and cell signaling techniques to better understand and utilize this stem cell populations.
